By Masooma Hyder Baig
Introduction
Psychological stress is a factor everyone will experience at multiple points during their lifetime. It can occur when individuals are placed under mental, physical or emotional pressure or multiple pressures that they may perceive to exceed their capacity (Chen and Lyga, 2014). In response to stress, one may experience different physiological and behavioural changes as the body tries to adapt. This article explores the physiological changes that can occur when experiencing stress.
Skin Structure and Normal Function
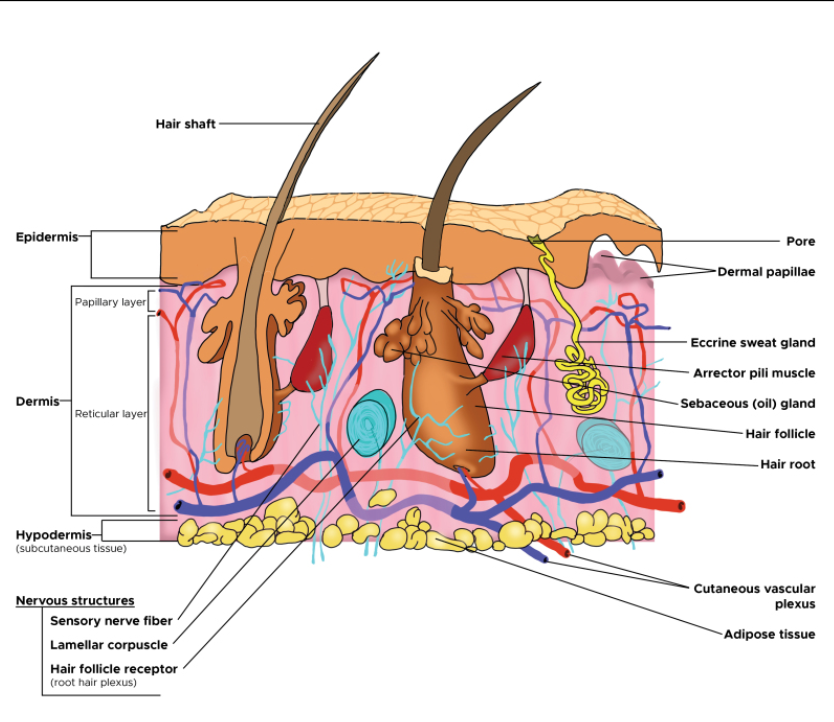
The skin consists of three layers: the epidermis, dermis and hypodermis. The epidermis additionally consists of multiple cells which include but are not limited to keratinocytes and melanocytes. Keratinocytes are found in the basal layer of the epidermis and produce keratin, secretes lipids to form the epidermal water barrier and regulates calcium absorption. Melanocytes are found between cells of the stratum basale of the epidermis and produce melanin which is a pigment that gives skin its colour and protects it from UV radiation (Yousef, Alhajj and Sharma, 2020). The dermis lies underneath the epidermis and is composed of elastic collagen fibres which allow the skin to stretch, capillaries to supply cells with oxygen and nutrients, sensory cells and sweat glands (Institute for Quality and Efficiency in Health Care, 2016). The final layer is the hypodermis (also referred to as the subcutaneous layer) which contains fat lobules, hair follicles, sensory neurons and blood vessels.
The skin has a plethora of functions to maintain the body’s homeostasis. It acts as a barrier to water, pathogens and UV rays. Sensory receptors detect pain (nociceptors), Pressure (mechanoreceptors) and temperature (thermoreceptors) enabling the skin to send signals to the brain allowing it to act as a sensory organ. It regulates body temperature through sweat and plays a role in immunity by interacting with the immune system (Yousef, Alhajj and Sharma, 2020).
Stress-Induced Inflammation
The skin-brain axis is often involved in the way psychological stress manifests in the skin. Stressful experiences lead to the body triggering the hypothalamus-pituitary-adrenal (HPA) axis which are three glands that play a major role in the body’s fight or flight response (Nathan, 2021). The stimulation of these glands leads to the production of hormones called catecholamines which are pro-inflammatory factors that lead to the activation of various inflammatory factors including cytokines IL-6 and IL-10 (Gubbi et al., 2020). Additionally, stress leads to the release of cortisol from the HPA axis which can result in mast cell stimulation – further increasing skin inflammation (Kempuraj et al., 2019). This can result in the exacerbation of conditions like psoriasis, atopic dermatitis, alopecia areata and erythema (Chen and Lyga, 2014).
Barrier Function and Wound Healing
Psychological stress can also disrupt epidermal barrier function by initiating a decrease in the production of epidermal lipids and structural proteins: vital for the barrier’s function of maintaining skin moisture levels and preventing microbes from entering the body. Overall these factors can also contribute to worsening skin conditions in addition to prolonging the skin barrier’s ability to repair (Nathan, 2021). Stress also leads to increased transdermal water loss, which weakens the barrier thus making the skin dry (Maarouf et al., 2019).
When stress causes excessive inflammation, it hinders the body’s ability to heal wounds where inflammation at the site of injury is a natural part of the body’s healing process (Gouin and Kiecolt-Glaser, 2011). Multiple studies have shown that stress plays a fundamental factor in delaying wound healing and dysregulating biomarkers associated with healing (Walburn et al., 2009). Furthermore, delayed wound healing has been proven to increase the chances of bacterial infections at those specific sites (Rojas et al., 2002) which could be associated with a decrease in antimicrobial protein expression caused by stress (Aberg et al., 2007).
Management
Thus, it becomes imperative for an individual to manage their stress to improve their overall skin health and well-being. The use of techniques like mindfulness, meditation, focused, deep breathing and cognitive behavioural therapy (CBT) can all contribute to aiding symptoms that come with stress. At the surface level, topical treatments that can either be prescribed by a healthcare professional or bought in-store could help restore the skin’s barrier and reduce stress-induced damage. Finally, lifestyle modifications to do with adequate sleep, frequent exercise, nature walks and changes in diet will all work to improve overall well-being and improve the look of skin.
Conclusion
To conclude, the skin is a complex organ, interconnected with multiple systems from immunity to the brain. These systems play prominent roles during times of psychological stress whether it be acute or chronic. Stress can induce prolonged inflammation, disruption to the skin barrier and delayed wound healing. This is largely through the activation of the HPA leading the the release of hormones like cortisol and catecholamines: putting the body in a state of fight or flight. This not only, exacerbates existing skin conditions but may compromise the body long-term if the underlying causes of stress are not dealt with. Thus, a combination of stress management, topical treatment and lifestyle changes can be adopted with advice from relevant healthcare professionals to ensure that action is taken to overall benefit the mind, brain, body and in turn skin.
Reference list
Aberg, K.M., Radek, K.A., Choi, E.-H., Kim, D.-K., Demerjian, M., Hupe, M., Kerbleski, J., Gallo, R.L., Ganz, T., Mauro, T., Feingold, K.R. and Elias, P.M. (2007). Psychological stress downregulates epidermal antimicrobial peptide expression and increases severity of cutaneous infections in mice. Journal of Clinical Investigation, 117(11), pp.3339–3349. doi:https://doi.org/10.1172/jci31726.
Chen, Y. and Lyga, J. (2014). Brain-Skin Connection: Stress, Inflammation and Skin Aging. Inflammation & Allergy-Drug Targets, 13(3), pp.177–190. doi:https://doi.org/10.2174/1871528113666140522104422.
Gouin, J.-P. and Kiecolt-Glaser, J.K. (2011). The Impact of Psychological Stress on Wound Healing: Methods and Mechanisms. Immunology and Allergy Clinics of North America, [online] 31(1), pp.81–93. doi:https://doi.org/10.1016/j.iac.2010.09.010.
Gubbi, S., Nazari, M.A., Taieb, D., Klubo-Gwiezdzinska, J. and Pacak, K. (2020). Catecholamine physiology and its implications in patients with COVID-19. The Lancet Diabetes & Endocrinology, 8(12), pp.978–986. doi:https://doi.org/10.1016/s2213-8587(20)30342-9.
Institute for Quality and Efficiency in Health Care (2016). How does skin work? [online] Nih.gov. Available at: https://www.ncbi.nlm.nih.gov/books/NBK279255/ [Accessed 20 Mar. 2024].
Kempuraj, D., Mentor, S., Thangavel, R., Ahmed, M.E., Selvakumar, G.P., Raikwar, S.P., Dubova, I., Zaheer, S., Iyer, S.S. and Zaheer, A. (2019). Mast Cells in Stress, Pain, Blood-Brain Barrier, Neuroinflammation and Alzheimer’s Disease. Frontiers in Cellular Neuroscience, 13. doi:https://doi.org/10.3389/fncel.2019.00054.
Maarouf, M., Maarouf, C.L., Yosipovitch, G. and Shi, V.Y. (2019). The impact of stress on epidermal barrier function: an evidence‐based review. British Journal of Dermatology, 181(6), pp.1129–1137. doi:https://doi.org/10.1111/bjd.17605.
Nathan, N. (2021). Stress May Be Getting to Your skin, but It’s Not a one-way Street. [online] Harvard Health. Available at: https://www.health.harvard.edu/blog/stress-may-be-getting-to-your-skin-but-its-not-a-one-way-street-2021041422334 [Accessed 20 Mar. 2024].
Rojas, I.-G., Padgett, D.A., Sheridan, J.F. and Marucha, P.T. (2002). Stress-Induced Susceptibility to Bacterial Infection During Cutaneous Wound Healing. Brain, Behavior, and Immunity, 16(1), pp.74–84. doi:https://doi.org/10.1006/brbi.2000.0619.
Walburn, J., Vedhara, K., Hankins, M., Rixon, L. and Weinman, J. (2009). Psychological stress and wound healing in humans: A systematic review and meta-analysis. Journal of Psychosomatic Research, 67(3), pp.253–271. doi:https://doi.org/10.1016/j.jpsychores.2009.04.002.
Yousef, H., Alhajj, M. and Sharma, S. (2020). Anatomy, Skin (Integument), Epidermis. [online] PubMed. Available at: https://www.ncbi.nlm.nih.gov/books/NBK470464/ [Accessed 20 Mar. 2024].
Yousef, H., Alhajj, M. and Sharma, S. (2022). [Figure, Cross section of layers of Skin]. [online] http://www.ncbi.nlm.nih.gov. Available at: https://www.ncbi.nlm.nih.gov/books/NBK470464/figure/article-21212.image.f2/?report=objectonly [Accessed 20 Mar. 2024].

Leave a comment